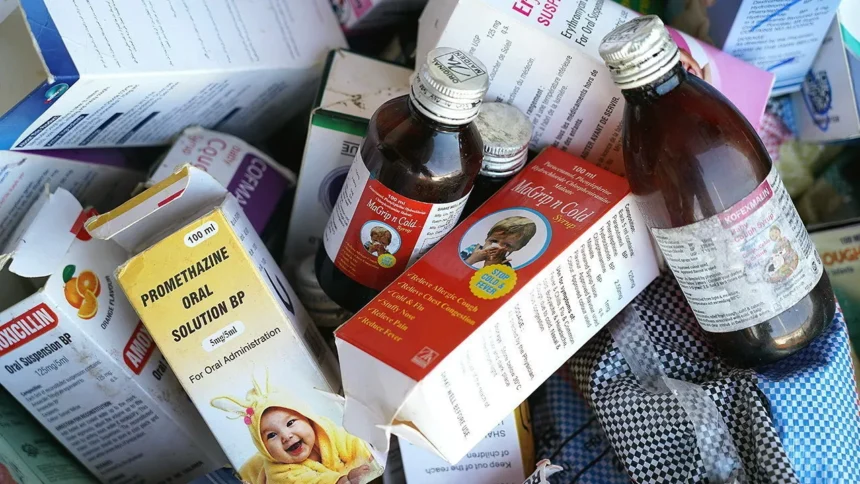
India’s pharmaceutical sector is reeling as safety lapses in cough-syrup manufacturing and oversight raise hard questions about drug exports. At least 20 children under five have died after ingesting contaminated syrups, triggering regulatory and reputational fallout for a once-proud export industry.
Contamination crisis grips pharma-exports image
The crisis began when doctors in a central Indian state reported multiple child deaths linked to the syrup brand “Coldrif”. Laboratory tests revealed the presence of diethylene glycol (DEG) in the syrup at levels hundreds of times above permissible limits. The syrup was manufactured by a Tamil Nadu-based company that had not upgraded its facility to the latest standards. Investigations uncovered that a chemical solvent (propylene glycol) had been sourced from a non-pharma grade distributor and may have been contaminated prior to use.
Weak oversight and regulatory holes undermine quality
India’s drug regulator has acknowledged that manufacturers failed to perform mandatory batch testing of raw materials and finished products. The pharmaceuticals industry regulation is fragmented between central and state agencies, which has contributed to inconsistent enforcement of Good Manufacturing Practices (GMP). Inspectors found factories where equipment hygiene, solvent storage and certification of ingredients were inadequately managed. The scandal highlights that regulatory oversight, particularly for generic exports, remains vulnerable.
Export implications and global market trust at stake
India’s pharmaceutical industry is a major global supplier, especially of generics and over-the-counter medicines. While recent statements indicate that the contaminated syrups were not officially exported, global watchdogs warn that unregulated supply channels may still have distributed them abroad. The reputational damage echoes prior events where Indian syrups were linked to child deaths in Africa and Central Asia. Export markets are now likely to demand stricter certification, audits and traceability from Indian manufacturers.
Policy and industry reaction signal change ahead
In response, the regulatory authority has ordered major upgrades of manufacturing facilities within a defined timeline. Smaller manufacturers have been given no extension after lobbying for delay. The government is also considering mandatory pre-export testing of high-risk medicines and tighter controls on ingredient sourcing. For the industry, firms are reassessing their supply chain risk, ingredient provenance and ethical audit frameworks to maintain access to sensitive export markets.
Takeaways
- Contaminated cough syrups in India caused child deaths and revealed major manufacturing and oversight failures.
- Manufacturers failed mandatory raw-material and batch testing; regulatory enforcement was inconsistent.
- India’s pharma-export credibility is under pressure; global buyers may demand stricter audits and traceability.
- The government is enforcing factory upgrades and considering enhanced pre-export testing for medicines.
FAQs
Q: What exactly was wrong with the cough syrups?
A: The syrups contained diethylene glycol (DEG), a toxic industrial solvent, at levels far above safety thresholds, due to use of sub-standard ingredients or solvents not meant for pharma use.
Q: Were these syrups exported internationally?
A: Officially the contaminated syrups were not exported. However, concerns remain that unofficial channels could have distributed them abroad, putting export credibility at risk.
Q: How is the regulatory system responding?
A: Regulators have ordered manufacturing plant upgrades, shut down offending units, suspended certifications and are pushing stricter testing and oversight, especially for export-bound products.
Q: What does this mean for India’s pharmaceutical industry?
A: The incident undermines trust in India’s status as a “pharmacy of the world”. The industry will face higher compliance costs, tighter export scrutiny and potential market access hurdles unless systemic reforms are enacted.